Prevent and Combat COVID-19 and Contagious Diseases in Corrections
Hi, I'm Ann Spalding and I am a public health physician. I've been trained in internal medicine and infectious disease. I have a Master's in Public Health from Johns Hopkins and I've been working in corrections since the mid-1990s.
Let's talk about prevention of COVID-19 in your correctional facility. So we've heard a lot of talk about the new Coronavirus. It is a Type B, which is more dangerous than the type A of Coronavirus that causes colds. The type B is like MERS and SARS and it causes much more severe disease. Let's talk about preventing this new disease from getting into your facility.
What's important about COVID-19 is screening and isolating. As we're talking about screening, we want to make sure that not only people who are coming into custody, but also people who work in a correctional setting will not be transporting this new virus into your facility.
There are three things that we'll be doing every day:

1. Make sure your staff is not coming in sick with fever, shortness of breath or cough. If somebody is sick as they report to work, they need to go home. You don't want somebody who should be at home on the job making everybody else who's working that day sick, making your population sick.
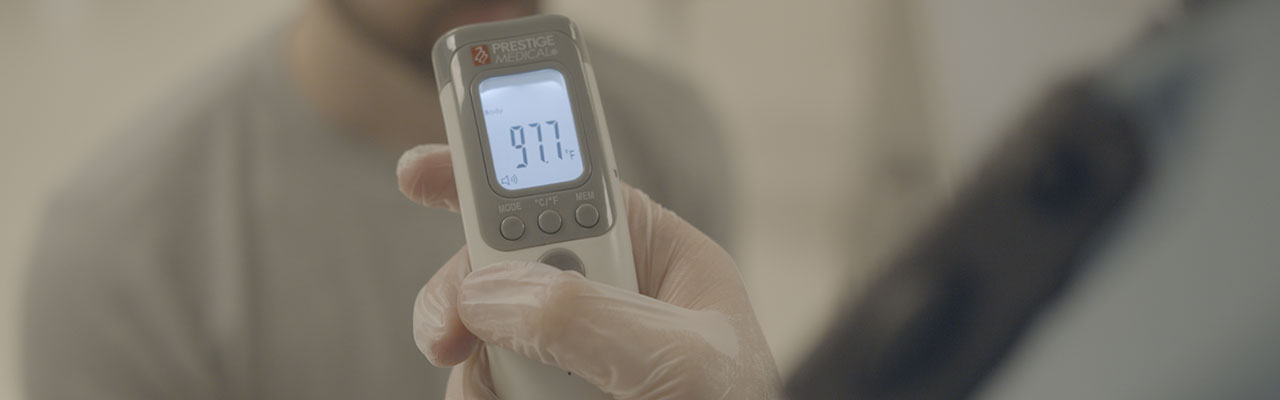
2. Screen offenders who are coming into custody to ensure they're not with fever, cough, and shortness of breath. Depending on your circumstances, you can take a temperature best. It's to have a no-touch means of taking a temperature. If the temperature is over a 100.4, you need to worry about the person.

3. Know about exposures of individuals before they come or have they been in an area where there is transmission ongoing in the community? Have they been exposed to cases on the outside prior to coming in?
A correctional facility, especially a small one with a limited staff, does not need medical personnel present 24/7 to ask important screening questions. Key questions include: Have you had significant exposure? Are you feeling sick? When individuals who are unwell arrive and staff cannot leave the building immediately, it is important to put a mask on that person. The type of mask we recommend is a surgical mask, not an N95 respirator. The sick individual should wear the surgical mask.
There may come a time when masks run low. If someone is coughing and does not have a mask, instruct them to cough into their elbow. Ensure that no one is coughing without covering their nose and mouth. Additionally, you should immediately remove that person from the general population to prevent further spread.
The best way to isolate someone who is sick is to place them in a negative pressure room. If a negative pressure room or bed space is unavailable, the next best option is a closed room. If there is a trap on the door, keep it closed rather than open. This helps contain the air inside and prevents it from infecting others.
Who should be transported out? Inmates who are unstable. Inmates who are likely to fare worse with this disease include those who are older and those with underlying medical conditions such as diabetes, high blood pressure, and heart disease. Inmates with underlying medical conditions and older individuals can deteriorate rapidly.
If community resources are not exhausted, a rescue can be called. An EMT should be contacted if those resources are unavailable. The safest way to transport someone is to ensure that the individuals conducting the transport have both distance and barriers in place.
The transporters should wear masks, ideally N95 masks, which can prevent particles and droplets from entering. However, even a surgical mask would be better than nothing. Additionally, the ill inmate should wear a surgical mask. If the windows are down, it will be safer than if they are up, so consider ensuring adequate air circulation in the vehicle. We want to keep individuals spaced as far apart as possible to maintain the health of our population.
Now is the time to consider video arraignments at the correctional facility instead of packing individuals into a van for transport. If possible, telemedicine evaluations should be utilized rather than bringing individuals to an outside healthcare facility, reducing the risk of exposing those who are not sick to potentially ill individuals.
Let’s discuss keeping your facility clean. We need to clean high-touch surfaces in the jail, including door handles, items that people push, and bars that people hold onto. These should be cleaned frequently with materials that can eliminate this virus. Look for hospital-grade disinfectants that are tested against coronaviruses; they will indicate effectiveness on the label. There is also evidence to suggest that household bleach, when diluted according to instructions, can work effectively. However, do not mix bleach with ammonia.
Another question that arises is how to clean a room after someone with COVID-19 or a high suspicion of it has occupied the space. We should allow time for air exchanges in that room before placing another individual in it.
The room should not be immediately available for use by another person. As of now, wait at least two hours before allowing another individual to enter. We should encourage those working in correctional facilities to stay informed about current events. We are in a people-oriented profession, constantly interacting with individuals, so it’s important to be aware of what’s happening nationally and in your community.
The bottom line during these times is to recognize our identity. We work in corrections and face threats and risks regularly; we meet these challenges and succeed. We have managed well in the past, and we can continue our good work. We can be thoughtful, proactive, and avoid panic.